Most people don’t wake up one morning and think, “Something is wrong with my brain.”
Instead, Cognitive Decline announces itself quietly.
It shows up as subtle changes you explain away: stress, aging, multitasking, menopause, burnout, poor sleep. And for a long time, those explanations feel reasonable. Until one day they don’t.
As a neurologist, I see this pattern every week. Highly intelligent, capable people come into my office saying, “I’m still functioning… but something feels off.” That moment matters. Early Cognitive Decline (including Mild Cognitive Impairment, or MCI) is often detectable, understandable, and, in many cases, reversible when addressed early.
This article is about what you notice first, why it matters, and what you can do now, long before a diagnosis ever enters the picture.
Early Cognitive Decline Signs Often Hides in Plain Sight

Source: https://dementia.stjohnsliving.org/dementia-warning-signs/
Cognitive decline rarely starts with dramatic memory loss. It usually shows up as small changes that feel easy to dismiss.
Common early signs include:
- Trouble finding familiar words
- Losing your train of thought while speaking
- Slower recall of names or recent conversations
- Mental fatigue from tasks that once felt easy
- Difficulty juggling multiple steps
- Feeling less sharp or mentally flat
Many people call this brain fog. Brain fog is not a diagnosis, but it is a signal. Symptoms may come and go at first, which is why people ignore them. Persistent changes deserve attention.
Studies suggest that these early changes often relate to cognitive aging rather than dementia, especially when addressed early.
Normal Aging vs Cognitive Decline
Aging does affect thinking and memory, but not all changes are normal. It helps to know the difference.
| Normal Aging | Possible Cognitive Decline |
| Occasionally forgetting names | Frequently forgetting recent events |
| Slower learning speed | Trouble following familiar steps |
| Misplacing items sometimes | Losing items and not retracing steps |
| Needing reminders | Relying heavily on notes for basics |
| Staying independent | Feeling less confident in daily tasks |
Cognitive decline may still allow independence, especially in people with mild impairment. The key difference is consistency and impact on daily life.
Mild Cognitive Impairment Deserves Serious Attention
Mild Cognitive Impairment (MCI) sits between normal aging and dementia. People with MCI are still independent. They’re still working, driving, managing finances, and living full lives.
But something has changed.
They may:
- Take longer to process information
- Need more reminders or notes
- Feel less confident in complex situations
- Notice others gently correcting or helping more than before
MCI is important because it is not destiny.
Some people with mild cognitive impairment progress to Alzheimer’s disease, while others remain stable for years. Long-term studies show that annual conversion rates from MCI to Alzheimer’s range from about 5 to 15 percent, depending on underlying pathology and risk factors. Importantly, not everyone declines. A meaningful portion of individuals with MCI either remain stable or show cognitive improvement, particularly when reversible contributors such as metabolic dysfunction, nutritional deficiencies, sleep disorders, or hormonal changes are identified and treated.
This is where timing matters.
Alzheimer’s Disease Starts Years Before Diagnosis
Here’s something most people don’t know:
Alzheimer’s disease has a long, silent phase(often 10 to 20 years) before a formal diagnosis is made.
During this subclinical period:
- Brain changes are already underway
- Neurons are under metabolic stress
- Inflammation and protein misfolding quietly accumulate
- Memory may still test “normal” on routine screening
By the time someone is told they have Alzheimer’s, the disease has usually been active for years, sometimes decades.
The good news? That long runway creates opportunity.
Blood Biomarkers and Early Brain Changes
New blood tests are changing how doctors evaluate cognitive decline. One important marker is p tau 217.
What p Tau 217 Tells Us
One of the most exciting advances in neurology is the ability to detect Alzheimer’s-related pathology early, using blood biomarkers.
Among these, p-tau 217 stands out.
- p-tau 217 reflects abnormal tau phosphorylation associated with Alzheimer’s disease
- It can be measured in blood (no spinal tap required)
- Elevations can appear years before symptoms become obvious
- It helps differentiate Alzheimer’s-type pathology from other causes of cognitive symptoms
This doesn’t mean that an elevated p-tau 217 level equals inevitable dementia. It means the brain is under a specific kind of stress, and that information allows earlier, more targeted intervention.
Many Causes of Cognitive Decline Are Treatable
Not all cognitive changes come from neurodegeneration. Many are linked to metabolic, hormonal, or nutritional issues.
Hormonal Changes and Brain Function
Source: https://lonestarneurology.net/others/how-hormonal-imbalances-impact-neurological-health/
Hormonal shifts, especially around midlife, can affect cognitive abilities. Many women notice sudden changes around menopause.
Common symptoms include:
- Word-finding difficulty
- Memory lapses
- Reduced mental stamina
In many cases, hormone replacement therapy (HRT) (appropriately prescribed and monitored) leads to rapid improvement in cognitive clarity.
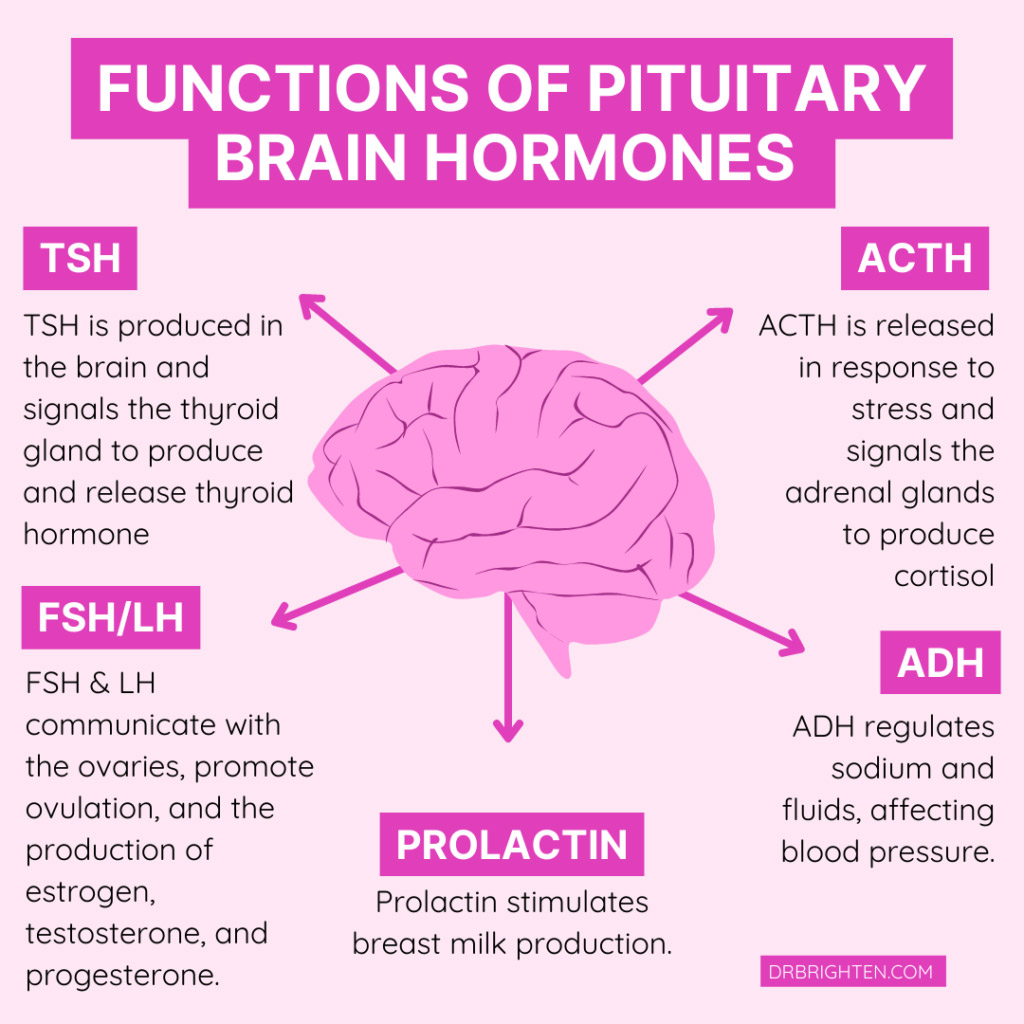
Source: https://drbrighten.com/brain-health-and-hormone-balance/
Vitamin D and Brain Health
Vitamin D supports immune regulation and brain signaling. Vitamin D plays a critical role in:
- Neuroimmune regulation
- Synaptic health
- Neuroprotection
Levels below optimal are associated with increased risk of Cognitive Decline.
In my practice, I aim for: Vitamin D levels above 50 ng/mL
This is not about megadosing. It’s about restoring a level that the brain expects for normal function.
Omega-3 Fatty Acids and Inflammation
The modern diet is heavily skewed toward omega-6 fatty acids, which promote inflammation.
The brain, however, thrives on omega-3s, particularly DHA.
Adequate omega-3 levels:
- Support neuronal membrane fluidity
- Reduce neuroinflammation
- Improve signaling efficiency
Balancing omega-6 with omega-3 intake is one of the simplest, most powerful steps you can take for cognitive health.
B Vitamins and Thinking Abilities
Low B12 or folate can cause cognitive symptoms that mimic dementia. Deficiencies in vitamin B12 and folate are common and often missed.
Low or suboptimal levels can cause:
- Memory problems
- Confusion
- Slowed thinking
- Depression and apathy
In some cases, correcting a B vitamin deficiency leads to marked cognitive improvement, particularly in individuals with vitamin B12 or folate deficiency, where treatment has been shown to reverse memory problems, confusion, and slowed thinking.
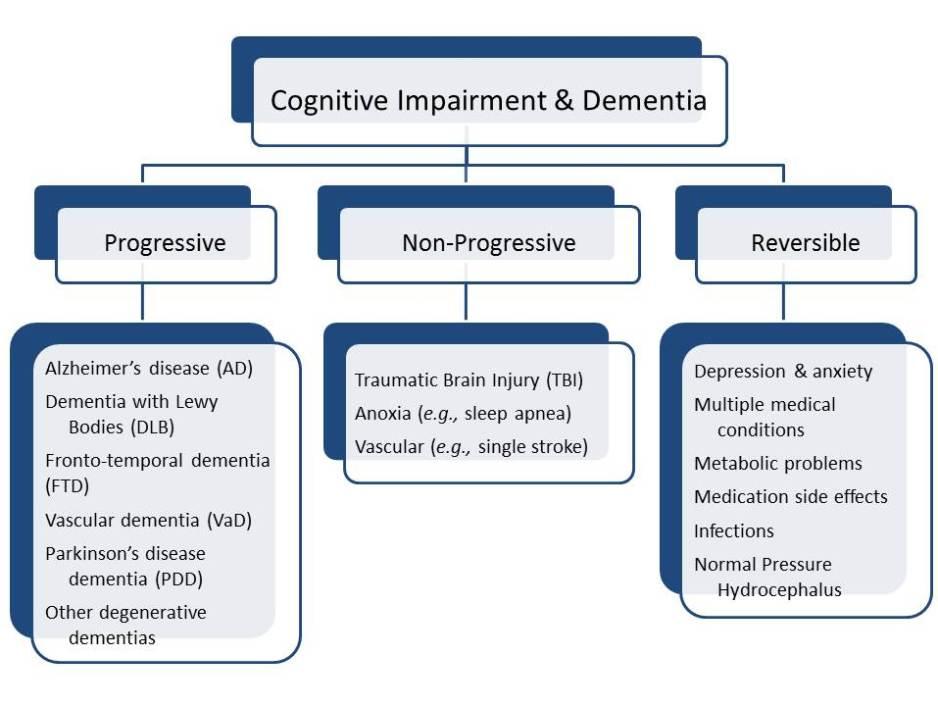
Source: https://mind.uci.edu/dementia/
Lifestyle Choices Shape Cognitive Aging
Your brain is the most metabolically demanding organ in your body. It is exquisitely sensitive to:
- Blood sugar instability
- Insulin resistance
- Inflammation
- Poor sleep
- Chronic stress
Dietary patterns that support cognitive resilience tend to:
- Stabilize glucose and insulin
- Reduce inflammatory load
- Provide micronutrient density
- Support mitochondrial function
Equally important:
- Regular physical activity
- Deep, restorative sleep
- Stress regulation
These are not generic wellness tips. They are biological interventions that influence cognitive trajectory.
Brain Fog Is a Clue, Not a Conclusion
Brain fog can come from many sources:
- Hormone imbalance
- Hearing loss
- Sleep apnea
- Thyroid issues
- Depression or anxiety
- Inflammation
- Early neurodegenerative change
The mistake is assuming it is either nothing or dementia. The right step is evaluation.
Why Early Action Changes Everything
The brain is plastic, adaptive, and responsive.
Early Cognitive Decline is often a state, not a fate.
When we:
- Identify contributors early
- Use modern biomarkers appropriately
- Address metabolic, hormonal, and nutritional drivers
- Implement targeted lifestyle interventions
We change trajectories.
I’ve seen people regain clarity, confidence, and cognitive stamina;not because they were lucky, but because they acted early.
What You Can Do Now
If you recognize yourself in this article, here are practical next steps:
- Take symptoms seriously (even if they’re subtle)
- Seek a comprehensive cognitive evaluation, not just a memory screen
- Ask about biomarkers, including p-tau 217 when appropriate
- Evaluate hormones, especially during midlife transitions
- Optimize vitamin D, omega-3s, B12, and folate
- Address sleep, stress, and metabolic health
Empowerment begins with information and action follows clarity.
Frequently Asked Questions
Is cognitive decline a normal part of aging?
Some changes with age are expected, but a persistent decline in thinking and memory is not. Cognitive decline may signal an underlying issue that deserves evaluation.
At what age do early signs usually appear?
Many people notice changes around age 45 to 65. Risk factors increase with age, but younger adults can experience symptoms too.
Can cognitive decline be reversed?
Some causes are reversible, especially in people with mild impairment. Hormones, nutrition, sleep, and metabolic health all play a role.
Does mild cognitive impairment always lead to dementia?
No. Some people remain stable for years. Others improve. Early assessment helps guide the outcome.
When should I see a specialist?
If symptoms persist, worsen, or affect daily life, schedule an evaluation at a medical center experienced in cognitive health.
Conclusion
Cognitive decline does not begin with dementia. It often starts with subtle changes such as difficulty finding words, mental fatigue, or persistent brain fog. These early signs are easy to dismiss, but they are also important clinical signals that deserve attention.
When cognitive changes are evaluated early, there are more options to understand what is happening and how to respond. Today’s diagnostic tools allow clinicians to assess risk factors, establish a baseline, and recommend evidence-based strategies that support long-term brain health.
If you have concerns about your memory, focus, or mental clarity, the next step is not to assume the worst. It is to get informed. A professional evaluation can provide clarity, guidance, and a plan tailored to your needs.
Schedule a consultation to discuss your symptoms and determine whether further assessment is appropriate. Early action is not driven by fear. It is guided by informed, proactive care.